As I embark on my journey of becoming a sex therapist, I learn more and more that without justice-justice there is no reproductive justice. We're fighting for them to take us serious at the doctor's in life or death matters, so how the f*ck do we get them to care enough to provide us with the proper information on contraception? The answer to this question is a lot more long-winded than we can get into right here and now, but what our sordid history with white supremacy at the intersection of medicine (especially in the reproductive realm) has taught us anything, it's simply this: be knowledgeable and aware of said history, then take that knowledge and demand what's best for your body and your choices.
My greatest recommendation is finding a doctor who looks like you if at all possible, but if that's not possible, here is the lowdown on one type of birth control that gynecologists and clinicians aren't talking about nearly enough and when they do, it seems to be disproportionately pushed on black and brown bodies in a way that can be "eerily" off putting — LARCs, or Long-Acting Reversible Contraception. I believe this is birth control info that everyone should have access to, so we're making it accessible!
This type of contraception lasts anywhere from three to twelve years, depending on which one you select and if you don't like it, it can be immediately removed pending a doctor's appointment. For those that are hormonal, the major implications of hormones will reverse almost immediately after removal in many cases. However, as always, it's worth mentioning that everyone's body is different and thus those results might be different.
LARCs fall under two categories: Intrauterine Device (two variations, one is nonhormonal) and the Implant.
No IOUs, Just an IUD
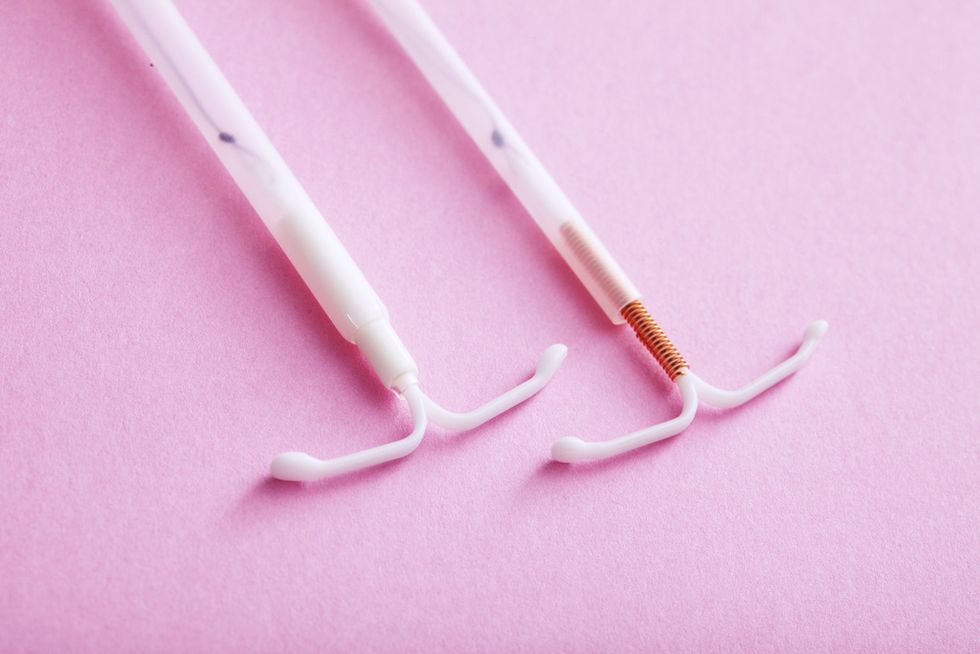 Method: IUD (Hormonal - Progesterone Only)Shutterstock
Method: IUD (Hormonal - Progesterone Only)ShutterstockSeemingly, the most commonly known LARC is an IUD. The IUD is a 't'-shaped piece of plastic that is inserted into the uterus as the name might imply. So with the copper IUD, that little 't' comes wrapped up in copper while the other forms of an IUD are plastic with a synthetic variation of progestin known as levonorgestrel shooting out like a battleship in a game of Galaga. With the copper IUD, it also acts as an alternative to over-the-counter emergency contraception and is most effective than if taken within five days (the sooner, the better) for those who thought they had a pullout game or simply had the misfortune of having a shitty condom.
You might have heard about this from older generations of women who experienced the horrors of the Dal-kon Shield, where the string from the IUD was causing infection in many women and a doctor continued to push them despite knowing this. Other physicians were never informed, as a result, women were deemed infertile in some cases and dead in others. This was during the 70s when the IUD rose to popularity in the US (despite being on the market since the 50s), it has since been remodeled to avoid these complications. As of today however, there are very rarely complications with IUDs. In fact, for some it has become the BFF of birth control.
For women who have contraindications for hormonal contraception, there is a nonhormonal option within this category of LARCs. It's a copper IUD by the name of Paragard. Paragard boasts about being the only of its kind in that is 100 percent hormone-free. You're probably asking yourself, well how can this birth control method effectively prevent pregnancy if there are no hormones involved? To keep it simple, sperm doesn't like copper so when the two cross paths, sperm scurries back away from the vaginal canal.
The other forms of IUDs, non-copper or hormonal IUDs, release progestin in order to thicken the cervical mucus and block eggs from crossing the barrier.
Eggplanted or Implanted
Nexplanon (formerly known as Implanon), or the implant contraceptive, work the same as hormonal IUDs in that they rely on progestin to create a barrier of mucus to keep eggs from traveling through. They are another form of long-acting reversible contraceptives and are inserted between the biceps and triceps. It takes on a simple shape as a small, plastic rod about the length of your pinky finger and the width of a sliver or a "matchstick." Both methods are 99 percent effective with typical use, making them more effective than any other method of birth control on the market.
As an FYI: typical use is the use outside of labs that takes into account user errors such as forgetting appointments, pills, etc that would dilute the effectiveness of birth control.
Unfortunately, they have a similarly deceptive and disappointing history to the Dal-kon shield with one of the first models of the implant to be popularized — Norplant. But even worse, the government pushed incentive during the 90s for women on welfare to get the implant inserted as a modern answer to the eugenics movements. These terrifying histories have created mistrust in even the most well-meaning physicians and rightfully so.
One Size Fits All
 Birth Control 101: Choosing The Best Contraceptive Method For You
Birth Control 101: Choosing The Best Contraceptive Method For YouThere are still some doctors who don't feel comfortable inserting IUDs into women who have yet to have children, according to them it is more of an uncomfortable insertion when the cervix has never been dilated in a big way. Then there are doctors who simply don't feel comfortable and this may or may not have to do with their own feelings towards it, implicit bias, or a lack of knowledge on their part. The reality is that the IUDs are slightly different in size and none of them are big or small enough to truly make a difference in the discomfort that has notably been associated with womanhood. To that effect, there is actually little to no pain associated with insertion of either of these devices, however, there can be quite a bit of bruising after having it inserted.
Also, what I will disclaim is that in removing the implant it requires the doctor to make a small incision. In some cases, the implant may move over time and may require a little more pressure to find and remove. Nonetheless, this pain is not even pain but more like I described before — discomfort. If ever you are unable to feel the implant in your arm, it's important that you make an appointment with your doctor.
Show Me the Money
The short-term cost of LARCs are hands down more pricey than that of other upfront cost for your barrier methods and your oral methods. But when we look at the long-term cost that includes transportation, prescription cost, etc over a lifetime it is far more cost effective to get a LARC. Still, I'm aware of the barriers that may be in the way of getting these methods, especially with the Trump administration. It goes without saying you should check with your insurance (Medicaid included), companies first to see if they cover LARCs but if not, there are resources such as Planned Parenthood that offer income-based payment options.
This was hugely important for me as someone whose insurance was funded through a Catholic organization, and I've had my implant funded through PP twice now. Without aid or insurance, the cost of LARCs can be hundreds of dollars, specifically ranging from about $400 to nearly $1000 (or more). Bedsider makes it easy for those who may not have insurance to check out local clinics that might offer these methods at low to no cost.
Here at xoNecole, we are not physicians and by no means are we suggesting that you go forward with this method without speaking to your gynecologist, namely to ensure there are no contraindications that might put you at risk when using a LARC. What we are suggesting is that women stay armed with knowledge and potential options that may work for their bodies, especially if we see that our own physicians are not providing this info. But especially as birth control is not a one size fits all band aid that they try to make it out to be by pushing certain methods on certain groups in the way I've seen and heard of them doing with Depo-Provera.
If knowledge is power, then I can't imagine the weapon we might become if we continue to push for knowledge that affords us true reproductive justice, as it allows us to do what we feel is best for our bodies for us to move through life comfortably.
While reproductive advances may have been created to eliminate our existence and reduce our right to bodily autonomy, you being informed is an act of resistance and you deciding what works for your body—well, that's us taking control in ways they never imagined—regardless of what we choose.
Featured image by Getty Images
Want more stories like this? Sign up for our newsletter here and check out the related reads below:
My Complicated Relationship With Safe Sex
Why I Quit Birth Control And Never Looked Back
Who Said That?! The Biggest Myths About Birth Control Explored
The 411 On The Morning After Pill
- Long-Acting Reversible Contraceptive Methods | HHS.gov ›
- Long-Acting Reversible Contraception | NEJM ›
- Understanding LARC | American Sexual Health Association ›
- Long-acting reversible contraception ›
- Long-Acting Reversible Contraception (LARC) - Your Guide ›
- Long-Acting Reversible Contraception Program - ACOG ›
- Long-acting reversible contraception - Wikipedia ›
- Long-Acting Reversible Contraceptives (LARCs) | Planned ... ›
- Long-Acting Reversible Contraception: Implants and Intrauterine ... ›
- Long-Acting Reversible Contraception | Planned Parenthood Mar ... ›